Image-guided radiation therapy
Radiation therapy is an essential part of the treatment for several cancers
Radiation therapy is a type of cancer treatment that uses intense energy beams for local treatment of tumors. Most types of radiation therapy use photon beams (X-ray or gamma-ray), but also Proton-beam therapy or other types of particle energy sources can be used.
The high energy beams used in radiation therapy treat cancer by destroying the genetic material that controls how the cancer cells grow and divide.
Photon beam radiation therapy has shown to be the most cost-effective treatment option for many cancer types, and approximately 50% of all cancer patients receive radiation therapy as part of their treatment regimen1,2.
In clinical practice, radiation therapy can be proposed at different times in the course of a cancer disease and for different reasons, including:
- As the primary treatment with curative intent, either as stand-alone or in combination with chemotherapy
- To shrink a cancer tumor before surgical removal (neoadjuvant radiation therapy)
- After surgery to destroy remaining cancer cells (adjuvant radiation therapy)
- To alleviate symptoms from the tumors and prolong life in advanced cancer cases (palliative therapy)
External beam radiation therapy
Radiation therapy can be delivered by an external beam or by an internal source. Internal radiation is referred to as brachytherapy and outside the scope of this section.
External beam radiation therapy is typically prescribed to a cancer patient as daily treatment fractions delivered over four to eight weeks, with the rate and time span of the treatment depending on the reason for this choice of therapy (see the section above).
During a fraction of external radiation treatment, the high-energy beam is delivered from a device outside the patient and targeted the tumor area inside the patient.
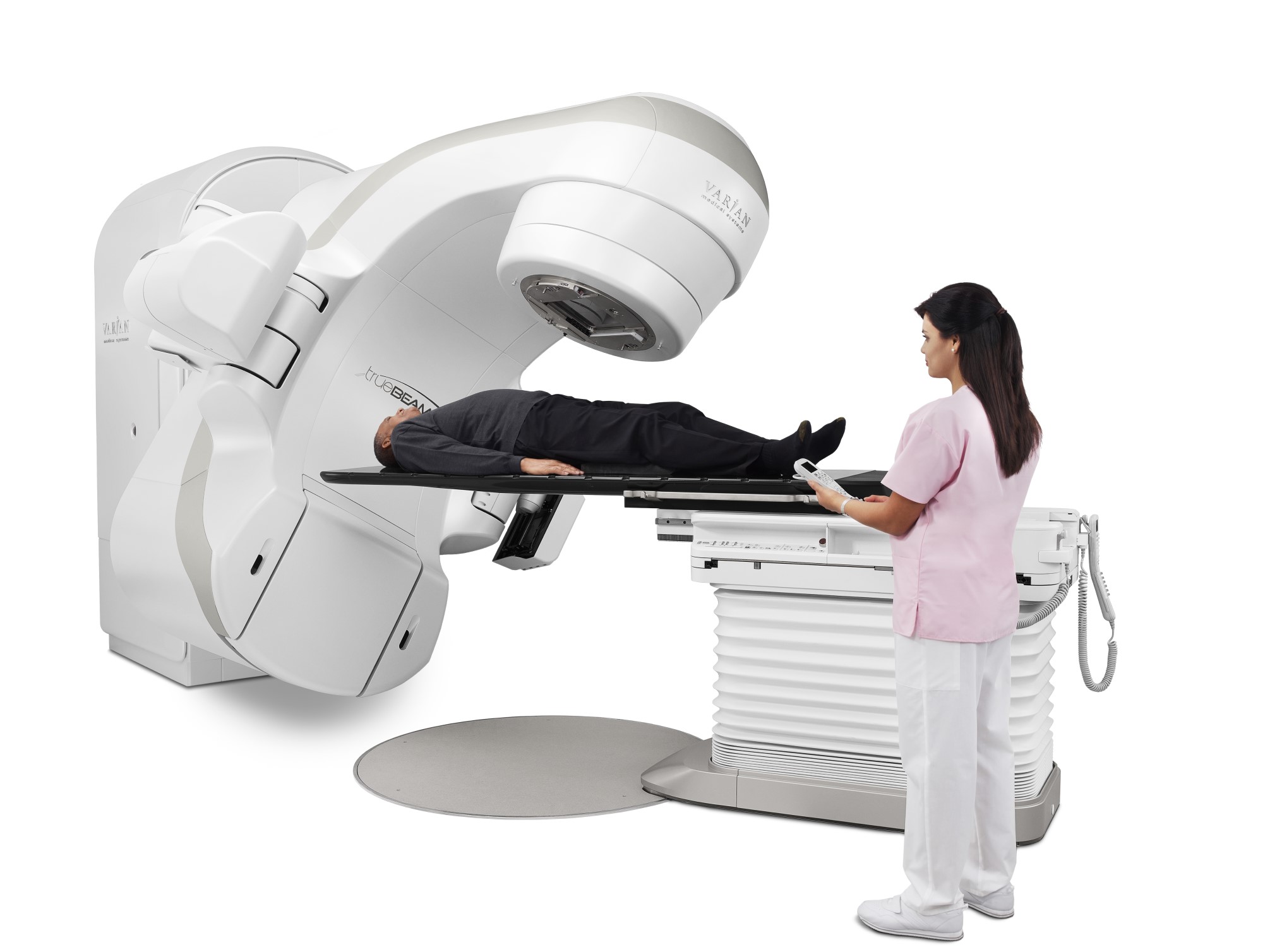
Image courtesy of Varian Medical Systems, Inc. All rights reserved.
The importance of high precision
Photon beam radiation causes cell damage to a tumor as well as the surrounding healthy tissue. The cellular damage of the radiation increases with the dose of energy deposited in the tissue.
Because of the harmful effect of photon radiation on healthy tissue, the delivery of lethal tumor doses is not always possible. The risk of unwanted radiation-induced damages to critical healthy tissue and organs must be taken into consideration.
The aim of radiation therapy is therefore to maximize the dose (and damage) delivered to the target tumor while minimizing the radiation outside the target and thereby reducing the risk of damage to healthy tissues.
In other words, the ability to target the energy beam with high precision to the tumor is crucial for the therapeutic outcome of the cancer treatment in terms of both efficacy and side-effects.
High precision radiation therapy is however challenging in regions of the body where target organs are located deep and/or are prone to movement, including the lungs, esophagus, bladder, rectum, liver, pancreas, stomach and prostate gland, and critical also for the treatment of tumors located close to essential organs and tissues.
Image guided radiation therapy (IGRT)
Image guided radiation therapy (IGRT) is the use of frequent imaging of the target area immediately before and during each treatment fraction to improve the precision of the therapy.
To deliver radiation therapy with image guidance, the treatment unit must have equipment with onboard imaging capabilities that can generate images of the patient’s bony or soft-tissue anatomy in the treatment position. The imaging modalities are most often X-ray, including kV, fluoroscopy, Computed Tomography (CT), and cone beam CT (CBCT), but can also be magnetic resonance imaging (MRI).
IGRT allows the radiotherapist to better localize the target area and direct the radiation beam to the tumor immediately before or even during treatment delivery. Any necessary adjustments can be made to the patient’s position and/or to the radiation beams in order to precisely target the tumor and minimize radiation damage to healthy surrounding tissue.
The benefits of IGRT includes:
- Increased accuracy of radiation treatment
- Improved definition, localization and monitoring of target position and movements before and during treatment
- The possibility of higher, targeted radiation dosage to improve tumor control
IGRT requires good visibility on imaging of tumors and organs at risks. Organs and soft tissue tumor targets are however in many cases not clearly visible on x-ray images due to a very low tumor to tissue contrast ratio. To support IGRT, fiducial markers with high visibility can be implanted in proximity to, or in, the tumor prior to the radiation treatment to act as surrogates for an optimal patient set-up and to support high precision radiation treatment. See The role of fiducial markers for more information.
References
1. Grau C, Defourny N, Malicki J, Dunscombe P, Borras JM, Coffey M, Slotman B, Bogusz M, Gasparotto C, Lievens Y, Kokobobo A, Sedlmayer F, Slobina E, Feyen K, Hadjieva T, Odrazka K, Eriksen JG, Jaal J, Bly R, Chauvet B, Wil-lich N, Polgar C, Johannsson J, Cunningham M, Magrini S, Atkocius V, Untereiner M, Pirotta M, Karadjinovic V, Levernes S, Skladowski K, Trigo ML, Šegedin B, Rodriguez A, Lagerlund M, Pastoors B, Hoskin P, Vaarkamp J, Soler RC. Radiotherapy equipment and departments in the European countries: Final results from the ESTRO-HERO survey. Radiotherapy and Oncology. 2014 Aug;112(2):155–64.
2. INTERNATIONAL ATOMIC ENERGY AGENCY, Introduction of Image Guided Radiotherapy into Clinical Prac-tice, Human Health Reports No. 16, IAEA, Vienna (2019).